Understanding Peri-Implantitis : Causes, Symptoms, and Treatment
What is Peri-Implantitis?
Peri-implantitis is a dental condition characterized by inflammation and infection of the tissues surrounding a dental implant..
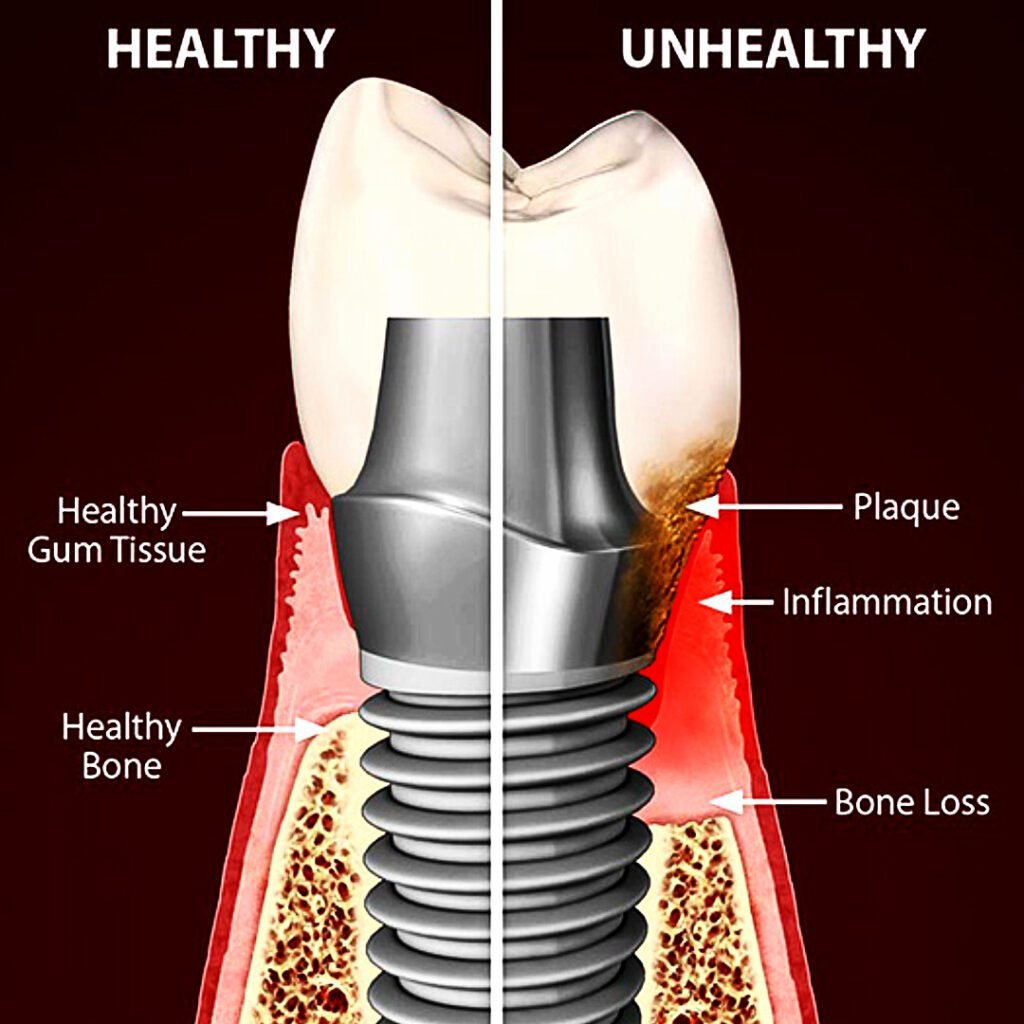
Peri-implantitis is a destructive inflammatory condition it affects the soft and hard tissues surrounding dental implants. The soft tissues become inflamed whereas the hard tissue (alveolar bone), which surrounds the implant for retaining it, is lost over time
Dental bridge can be made up of materials ranging from metal, ceramic, zirconia and even acrylic in some cases.
What Causes Peri-Implantitis?
Peri-implantitis may arise due to poor oral hygiene, smoking, diabetes, or a history of periodontal disease, leading to symptoms such as bleeding gums, bad breath, and looseness of the implant..
- Poor oral hygiene
- Smoking
- Diabetes
- History of periodontal disease
- Excessive biting forces on the implant
- Inadequate bone support around the implant
- Systemic diseases compromising immune function
- Genetic predisposition to inflammation
- Overloading of the implant during the healing phase
- Improper placement or angulation of the implant
- Presence of subgingival cement remnants after restoration placement
- Trauma to the peri-implant tissues during surgical or prosthetic procedures
These factors can contribute to the development and progression of peri-implantitis, leading to inflammation, infection, and potential loss of the dental implant.
How is Peri-Implantitis treated?
Treatment approaches vary based on the severity of peri-implantitis and may include non-surgical methods such as scaling and root planing, as well as surgical interventions like flap surgery or bone grafting.
Types of Treatment Available
- Non-Surgical Treatment:
- Scaling and Root Planing: Similar to treatment for gum disease, this procedure involves deep cleaning of the implant surface and surrounding tissues to remove bacterial plaque and calculus.
- Antimicrobial Therapy: Administration of antimicrobial agents, such as antibiotics or antiseptic mouth rinses, to reduce bacterial colonization and inflammation.
- Surgical Treatment:
- Flap Surgery: Involves lifting the gum tissue to access the implant surface for thorough cleaning and removal of diseased tissue. It may also include bone grafting to regenerate lost bone support.
- Bone Grafting: Addition of bone graft material to augment bone volume and support around the implant, promoting tissue regeneration and stabilization.
- Implant Surface Decontamination:
- Laser Therapy: Utilization of lasers to decontaminate the implant surface and surrounding tissues, targeting bacterial biofilm while minimizing damage to healthy tissue.
- Air Abrasion: Mechanical removal of microbial biofilm from the implant surface using abrasive particles propelled by compressed air or gas.
- Guided Bone Regeneration (GBR):
- Membrane Placement: Placement of barrier membranes around the implant site to prevent soft tissue ingrowth and promote bone regeneration in defect areas.
- Removal of Failing Implants:
- In cases of severe peri-implantitis with extensive bone loss and implant failure, removal of the implant may be necessary to prevent further complications and promote healing.
Each type of treatment aims to address the underlying infection, inflammation, and bone loss associated with peri-implantitis, with the goal of preserving the implant and supporting tissues while restoring oral health and function.
How is Peri-Implantitis Treatment Done
The choice of treatment depends on the severity of the condition, patient’s overall health, and individual treatment goals. It’s essential for patients to consult with a dental professional for proper diagnosis and personalized treatment planning.
Before the Procedure
Patients is advised to discontinue smoking, maintain good oral hygiene, and adhere to any prescribed medications to prepare for treatment.
During the Procedure
Treatment typically involves thorough cleaning of the implant surface and surrounding tissues to remove bacterial deposits and promote healing.
After the Procedure
Patients are instructed to follow strict oral hygiene practices, use prescribed antimicrobial mouthwashes, and attend regular follow-up appointments to monitor healing and prevent recurrence.
Typical Recovery Time
Recovery time varies depending on the extent of treatment but may range from a few weeks to several months.
Risks and Benefits of Peri-Implantitis Treatment
Risks: Risks associated with peri-implantitis treatment include infection, implant failure, and potential damage to surrounding tissues.
Benefits: Treatment aims to halt the progression of peri-implantitis, preserve the implant, and restore oral health and function.
Peri-Implantitis Precautions & Care
Patients should adhere to post-operative instructions, avoid smoking, maintain good oral hygiene, and attend regular dental check-ups to minimize the risk of peri-implantitis recurrence.
Long-Term Care
- Maintain Excellent Oral Hygiene:
- Brush teeth at least twice daily using a soft-bristled toothbrush and fluoride toothpaste.
- Floss or use interdental brushes to clean between teeth and around implants.
- Rinse with an antimicrobial mouthwash to reduce bacterial colonization.
- Attend Regular Dental Check-ups:
- Schedule routine dental examinations and cleanings with a dental professional.
- Regular monitoring allows early detection of peri-implantitis or other oral health issues.
- Avoid Smoking:
- Smoking increases the risk of peri-implantitis and implant failure by compromising blood flow and weakening the immune system.
- Quitting smoking or avoiding tobacco products can significantly improve implant success rates.
- Control Systemic Diseases:
- Manage systemic conditions like diabetes, which can impact healing and increase susceptibility to infections.
- Maintain optimal blood sugar levels through diet, exercise, and medication as prescribed by a healthcare provider.
- Protect Implants from Trauma:
- Avoid habits like teeth grinding (bruxism) and chewing on hard objects that can exert excessive force on implants.
- Use a nightguard if bruxism is a concern to prevent damage to implants and surrounding tissues.
- Follow Post-Operative Instructions:
- Adhere to any post-operative care instructions provided by the dental professional, including medication usage and dietary restrictions.
- Attend follow-up appointments as recommended for monitoring and adjustment of treatment if needed.
- Maintain Healthy Lifestyle Habits:
- Eat a balanced diet rich in nutrients to support overall health and immune function.
- Limit alcohol consumption, as excessive alcohol intake can impair healing and increase inflammation.
- Stay Informed and Educated:
- Stay updated on proper oral hygiene techniques and implant care guidelines provided by dental professionals.
- Seek professional advice if experiencing any unusual symptoms or changes around implants.
What Happens If You Opt for No Peri-Implantitis Treatment?
Choosing not to undergo peri-implantitis treatment can have several consequences, both in the short term and the long term. Here are some potential outcomes:
- Implant failure and potential loss: Untreated infection can lead to the loosening and eventual failure of the dental implant.
- Significant bone loss around the implant site: Infection causes deterioration of the supporting bone, compromising implant stability.
- Compromised oral function and esthetics: Gum recession and implant mobility can impact chewing ability and smile aesthetics.
- Chronic pain, discomfort, and sensitivity: Untreated inflammation can result in persistent oral discomfort and sensitivity.
- Increased risk of systemic health issues: Oral infections may contribute to systemic conditions like cardiovascular disease and diabetes.
- Higher complexity and cost of future interventions: Delayed treatment may necessitate more extensive and costly procedures in the future.
Ultimately, the decision to pursue treatment or not depends on individual circumstances, including oral health needs, budget, and personal preferences.
Cost of Peri-Implantitis Treatment
Cost Considerations: There is no ball-park figure for this but it can range between Rs 5000 – Rs 20000
Insurance Coverage: Some dental insurance plans may cover a portion of the cost, particularly if the procedure is deemed medically necessary. Patients are encouraged to check with their insurance provider to determine coverage options and any out-of-pocket expenses.
Frequently Asked Questions About Dental Bridge
[su_accordion]
[su_spoiler title=”What causes peri-implantitis?” style=”fancy”]
Peri-implantitis is primarily caused by bacterial infection and inflammation around dental implants, often due to poor oral hygiene, smoking, or pre-existing periodontal disease.
[/su_spoiler]
[su_spoiler title=”How do I get rid of peri-implantitis?” style=”fancy”]
Treatment for peri-implantitis typically involves thorough cleaning of the implant surface, removal of bacterial biofilm, and in severe cases, surgical intervention to repair or remove the implant.
[/su_spoiler]
[su_spoiler title=”What is the early stage of peri-implantitis?” style=”fancy”]
The early stage of peri-implantitis may manifest as bleeding gums, inflammation around the implant, or increased pocket depths on probing.
[/su_spoiler]
[su_spoiler title=”What is the case definition of peri-implantitis?” style=”fancy”]
Peri-implantitis is defined as inflammation and infection of the tissues surrounding a dental implant, often accompanied by bone loss and clinical signs of disease.
[/su_spoiler]
[su_spoiler title=”Can peri-implantitis be cured with antibiotics?” style=”fancy”]
While antibiotics may help control bacterial infection, they are typically used as adjunctive therapy alongside mechanical debridement and surgical intervention for treating peri-implantitis.
[/su_spoiler]
[su_spoiler title=”What is non-surgical treatment for peri-implantitis?” style=”fancy”]
Non-surgical treatment for peri-implantitis may include scaling and root planing, antimicrobial therapy, and adjunctive use of local antimicrobial agents or laser therapy.
[/su_spoiler]
[su_spoiler title=”What is the success rate of peri-implantitis treatment?” style=”fancy”]
The success rate of peri-implantitis treatment varies depending on the severity of the condition, treatment approach, and patient factors, but studies have reported success rates ranging from 50% to 90%.
[/su_spoiler]
[su_spoiler title=”How long does peri-implantitis take?” style=”fancy”]
The duration of peri-implantitis treatment varies depending on the severity of the condition, treatment approach, and individual healing response, but it may take several weeks to months to achieve resolution.
[/su_spoiler]
[su_spoiler title=”Can peri-implantitis spread?” style=”fancy”]
Yes, peri-implantitis can spread and affect neighboring implants or natural teeth if left untreated, leading to further complications and worsening of oral health.
[/su_spoiler]
[/su_accordion]
Dental Procedure Cost In Gurgaon
Explore the cost of dental procedures at our clinic in Gurgaon. For detailed information, visit: Dental Procedure Cost
Book Appointment with Best Dentist in Gurgaon
Schedule an appointment with our experienced dentists in Gurgaon. Click here to book: Book Appointment

Dr. Jyoti Singh (MDS), Diplomate WCOI (Japan region) Member AAID (American Association of Implant Dentistry) stands as a beacon of excellence in implantology within Delhi NCR region. She is a BDS and MDS(Prostho) both from Maulana Azad Institute of Dental Sciences, where she secured top honors with all India rank 1 in PG entrance examination. Her extensive experience at esteemed institutions like Clove Dental and her own Center for Dental Implants & Esthetics since 2016, Dr. Singh embodies unparalleled expertise in dental implants. Boasting a wealth of 17+ years in dentistry and backed by 18 groundbreaking research papers in leading international journals (Google Scholar) and her ResearchGate profile, she epitomizes the pinnacle of proficiency and innovation in her field. She practices in Gurugram as your friendly dentist near me.